
Holy MACRAoni!
Sadly, this article is not about the best macaroni and cheese recipe. The Medicare Access and CHIP Reauthorization Act (MACRA) of 2015 will soon change the payment methodology for medical practices. MACRA’s first performance year starts January 2017. Hopefully you have already started reading about the effects of MACRA in professional journals or by attending seminars and webinars; however, if this is the first time you heard about MACRA, now is the time to quickly become familiar with this change from the old Medicare physician fee-for-service payment system to a payment system based on patient value and outcomes.
MACRA produced three important changes to Medicare payments:
- Repealed the Sustainable Growth Rate (SGR) that plagued physician payments for years.
- Created a new payment system to reward physicians for quality, and not just for seeing the most patients.
- Combining existing quality measures into one system.
Physicians will choose to participate in either the Merit Based Incentive Payment System, known as MIPS, or the Alternate Payment Model, known as APM.
- MIPS will become a ‘modified fee for service’ payment system. Experts predict the majority of physicians will choose the MIPS payment model, which will be based on four factors: quality, cost, clinical practice improvement activities (care coordination), and advancing care information (EHR use). Each category will have a different weight in the calculation, and the weight factor will change over time.
- APM will consider quality and cost, which will include risk-based payments, similar to Accountable Care Organizations or Patient Centered Medical Homes. APM’s should increase the transparency of the physician-focused payment model. Those physicians choosing to participate in the APM model are exempt from participating in MIPS.
There are a small percentage of physicians who may be exempt from participating in these payment models, such as those physicians who treat less than 100 Medicare patients or receive less than $10,000.00 in Medicare payments each year; or those physicians in their first year of practice. The CMS website provides more information regarding the exemptions.
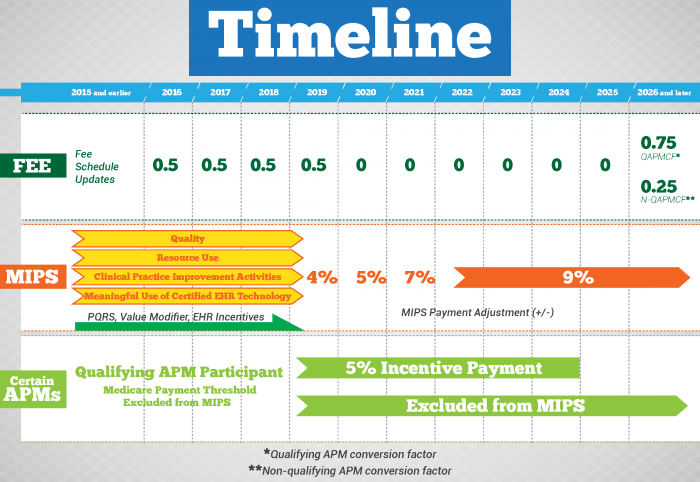
The timeline provides information regarding transitioning from the current Medicare payment system to the MIPS or APM payment models.
Physicians and medical practice managers must prepare for this change by becoming educated on the various payment models. The American Medical Association has several resources on their website to assist the practice with understanding and preparing for the MACRA changes. Physicians and medical practice managers can also contact their professional associations for information regarding MIPS and APM payment models, or refer to the CMS website. Just as we did for the ICD-10 transition, being prepared for this change will decrease the likelihood of revenue issues.
Several commercial insurance plans offer ‘risk based’ payment methodologies at this time, and once MACRA is implemented, we expect that trend to continue.
Contact Concordis Practice Management for assistance with the MIPS and APM transition.



No Comments